We have mentioned before about the predicament with completing ‘kegels’ (or the contraction phase of the kegel alone is what most end up doing). This has an inherent potential impact on labor and delivery.
Now there is new research out of the European Journal of Obstetrics & Gynecology and Reproductive Biology about the impact that there can be had when removing what is often referred to as ‘coached pushing’ during labor and delivery in addition to a few other key factors.
At Warman Physio we want to set women up for the best success possible during labor and delivery, and know that knowledge is power!
So let’s run through some of the background here.
The Facts From the Research
An article in Return to Now outlined the results from EJOG in a thought-provoking post. There is an 85% reduction in 3rd and 4th degree tears (the ‘worst’ of the available 1-4 scale) when women are not coached to push during labor. The amount of severe vaginal tearing was reduced from 7% to 1% within the study.
The researchers completed a review to determine what the main contributing factors were for third and fourth degree tears, and implemented a series of measures to try and reduce these risks.
Some of the risks include a larger than average baby, baby being born ‘face-up’, forceps use, previous perineal tear history, as well as maternal age and weight
This program is referred to as STOMP (Stop Traumatic OASIS Morbidity Project) and implemented within the hospital unit by the midwives and OB GYN teams over the following year. This program includes laboring in different positions to deliver the baby such as squatting, kneeling, and standing, as well as breathing through contractions instead of pushing and applying counter pressure to the perineum during delivery of the baby.
A total of 3902 vaginal deliveries occurred during the 1 year following the launch of full STOMP implementation, with the most significant and immediate results occurring in the first 5 months.
What Does This Mean?
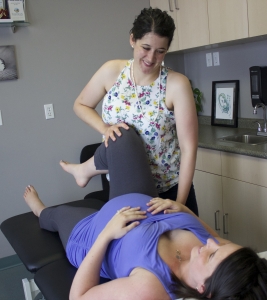
We have seen before in a video demonstration how the uterus does it’s job to push a baby out, coached pushing is shown to lead to closure of the perineum on the descending baby. Allowing women to follow their instincts, without coached pushing, is proven to reduce severe perineal tearing. This will not eliminate all perineal tearing, but gives additional information into how we can best support mothers during labor and delivery.
Physiotherapists are uniquely positioned to assist with mothers during this phase of life, particularly pelvic floor physiotherapists.
Although seeing a pelvic health physiotherapist is not the standard of care here in Canada, there are many women choosing to see one prior to labor and delivery for a variety of reasons such as leaking, pelvic pain, pain with intercourse, and low back pain or sciatica among others. There is also a large trend to see women post-natally as well due to the same reasons in addition to injuries sustained during labor and delivery such as perineal tears.
How can Physiotherapy Help?
Pelvic floor physiotherapists, like those we have at Warman Physio, are able to provide prenatal evaluation of the pelvic floor muscles, coordination, and information on labor and delivery preparation activities. Many women will have been practicing kegels throughout their pregnancy since there still is a significant amount of mis-information regarding what is ‘best’… (remember, a tight pelvic floor isn’t really what we are going for, a functional pelvic floor is what we want!)
In Saskatchewan women are provided an immediate referral to physiotherapy if they have received a third or fourth degree tear (which is GREAT!), however, any woman who has been pregnant into the second trimester may benefit from seeing a pelvic floor therapist after delivering baby.
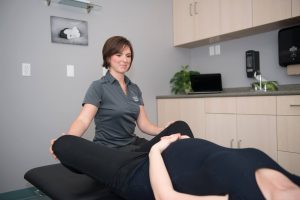
We have seen that in France, the standard of care is that every woman who has a baby is entitled to Pelvic Floor Physiotherapy appointments postpartum.
Reducing injuries during labor and delivery, and having research to support theoretical working knowledge is critical to advancing health and wellness for women of childbearing years.
Wonder if Physiotherapy can help you for labor and delivery? We recommend an appointment 32-34 weeks gestation. (For those with contraindications to a pelvic exam, we would complete various education and external assessment components).
Our Pelvic Health Therapists:


 We wouldn’t tell someone who has just started running that has developed knee pain that “this is just part of becoming a runner – it will go away when you stop
We wouldn’t tell someone who has just started running that has developed knee pain that “this is just part of becoming a runner – it will go away when you stop

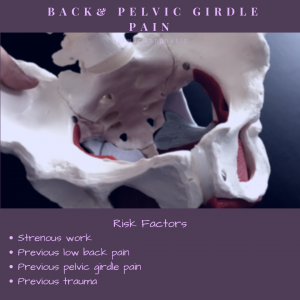
 What causes pelvic girdle pain?
What causes pelvic girdle pain?