It seems the topic of “Diastasis” is picking up speed in a variety of forums. Particularly on social media in mom groups and exercise discussions. There also appears to be a wide array of misinformation that continues to be spread around. I had one client tell me “I have been doing some research and one place I went to online said that if I have a diastasis I will ALWAYS look a minimum of 3 months pregnant.” This, for the vast majority, doesn’t necessarily need to be true; especially when you know what to do. I have been asked to write a few key things in regards to diastasis from a physiotherapy rehabilitation perspective.
…if I have a diastasis I will ALWAYS look 3 months pregnant
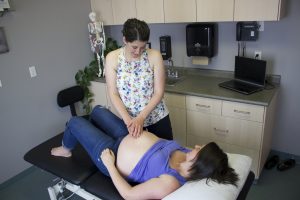
Let’s discuss what a diastasis is. The short version is it is the ‘splitting of the abdominal muscles’. A more specific answer is that in response to pregnancy, the abdominal muscles and associated tissue (fascia) stretch to allow room for a growing fetus. The muscles that are most affected by this is the rectus abdominis (the 6-pack ab muscles that sit in the front). This is not ‘bad’, cannot be prevented, and is in fact necessary during pregnancy. From a clinical perspective, I would say 100% of women who are pregnant, that look pregnant at the time of delivery, will have developed some diastasis during pregnancy. (Side note: diastasis can also occur outside of pregnancy, but that is another discussion.)
In theory, after labor and delivery, the diastasis will ‘snap’ back together and the core muscles will work in perfect unison… Sometimes this coordination comes naturally to women post-partum. However, often women require some help in getting all the pieces working well together in a functional and coordinated fashion.
…after labor and delivery, the diastasis will ‘snap’ back together
This is where people profit off our post-partum mommas “Get your body BACK after baby”, “Post-partum BOOTCAMP”, “Get rid of MUMMY TUMMY in 1 simple exercise”. Unless someone is checking for diastasis recti, do so on a regular (weekly, daily) basis, and can ensure that you are coordinating those muscles well… claiming to be a Post-Partum Specialist is likely an over statement. Often times I see that someone has “healed” their own diastasis and want to “show you how” with their main credential being that they went through the same thing, and they are fine after starting back into heavy exercise at “6” weeks post-partum.
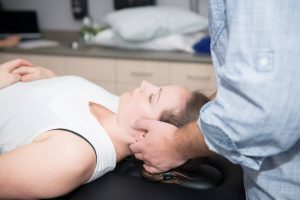
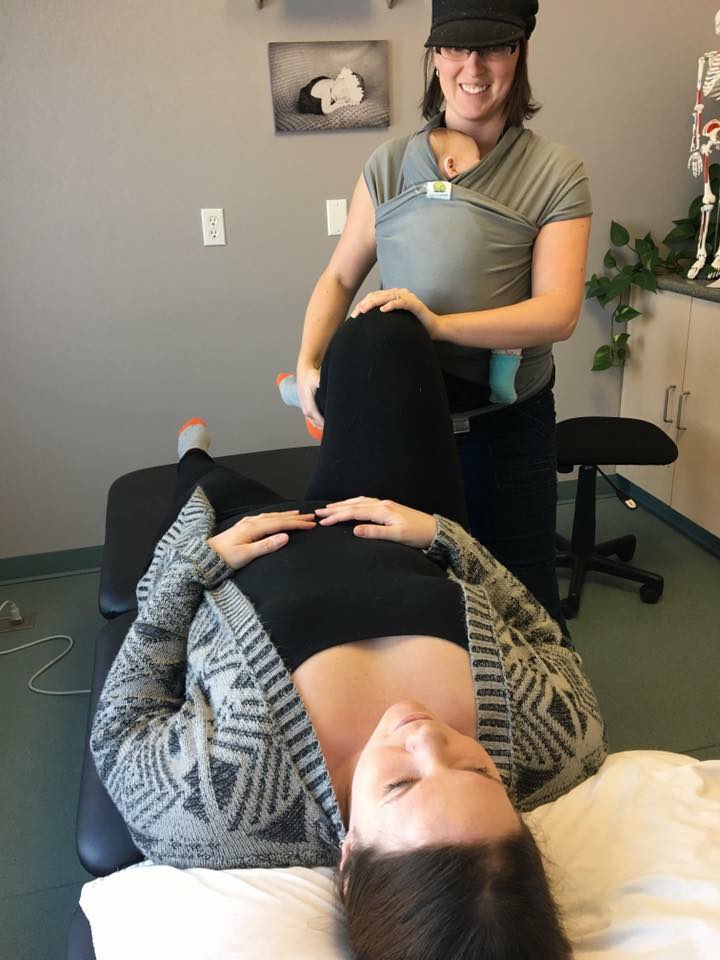
Simply asking people if they have a diastasis is not enough. Knowledge of the issue without being able to assist in modifying exercises to appropriately return to function is where many people stand. Are you wanting to start a class? Ask the instructor what they know about diastasis. If you don’t know if you have one, will they check? How many people have they checked? Not all postpartum fitness classes are created equal.
A diastasis is not necessarily a ‘quick fix’, and often people don’t realize they have it since it typically isn’t painful. What we do “know” is that a diastasis present at 8 weeks post-partum is likely to continue to be present (read dysfunctional) at a year post-partum. But what does ‘problematic’ mean if it’s not painful?
The tissue (fascia) of the diastasis doesn’t need to close in the sense of getting back to how it was, but it does need to be able to generate tension. If it can generate tension well and it is separated 2.5cm that person is going to have better function than if it is separated 1.5cm and not generating tension. (Think of tension as whether you have a firm uncooked noodle versus a soft, cooked noodle between the muscles. The cooked noodle will give away under pressure of the muscles on either side, and the uncooked noodle will hold and transfer force). Problematic could also be the contribution of diastasis to back pain, diaphragm dysfunction, and pelvic floor issues. Diastasis doesn’t cause these things, but it may contribute.
Focusing on the diastasis alone is a simplification of a complex situation, and each person will require slightly different treatment approaches.
What do I recommend? Contact your local pelvic floor physiotherapist, there is no time limit on when to go, but within the first 8-12 weeks will give time to get into a routine with baby and be early enough to have minimal “bad habits” or compensations to combat; or before you start back into exercise. It is never too late to address anything that has developed during pregnancy and post-partum.